Written by Greta Myers, DPT, NCS, CSRS, PWR! Moves Therapy & Certified Stroke Rehab Specialist
Article
Neurological, Stroke
 Stroke is the leading cause of serious, long-term disability in the United States, but a strong ‘Circle of Care’ after suffering a stroke, will help maximize your recovery. Your Circle of Care will likely consist of your physician, nurses and rehabilitation specialists like, physical, occupational, recreation, speech and language therapists, as well as mental health professionals. These providers are going to help you navigate through your recovery and your life after a stroke.
Stroke is the leading cause of serious, long-term disability in the United States, but a strong ‘Circle of Care’ after suffering a stroke, will help maximize your recovery. Your Circle of Care will likely consist of your physician, nurses and rehabilitation specialists like, physical, occupational, recreation, speech and language therapists, as well as mental health professionals. These providers are going to help you navigate through your recovery and your life after a stroke.
Physical therapy (PT) is a crucial piece of that Circle of Care. PT will support your neuromusculoskeletal concerns (the interaction between your brain, nerves, muscles and skeleton) for the rest of your life! It is typical for people with neurologic conditions to maintain long-term, intermittent relationships and communication with their physical therapist.1
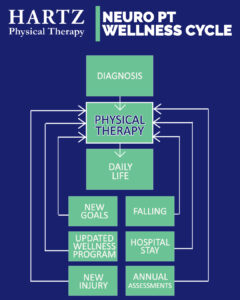
The importance of physical therapy for people with a neurological condition (including stroke) in the PT/Wellness Cycle cannot be underestimated. The journey towards recovery can be emotional, but your PT will help you maximize your functional abilities and your level of independence, as well as minimize the risk of further injury or medical problems.
Physical therapy probably started for you immediately after your stroke in the hospital. You may have then received physical therapy from another inpatient facility (i.e.: rehab, skilled nursing facility), and perhaps some home health physical therapy upon returning home. Finally, you should have transitioned to outpatient physical therapy which is where the PT/Wellness Cycle begins.
A recurring outpatient PT program will help you reach your goals after a stroke. Following up PT with a wellness plan including regular exercise, managing stress, improving nutrition, and caring for your mental health will help you further improve or maintain the gains you made in physical therapy and decrease the risk of secondary complications.
However, ‘graduating’ from therapy doesn’t mean it’s over! You should go back to physical therapy periodically if you experience any of the following:
• Increased falling
• Deterioration (feeling like you are unable to participate in activities as well)
• New goals (Specific activities you haven’t been able to do, but now want to work towards i.e., walking on the beach, gardening)
• Hospitalization
• New Injury
• Surgery
• Update wellness program (feeling like you plateaued with your current program)
Further, it is recommended that you have semi-annual or annual reassessments from your physical therapist.1 This allows you and the physical therapist to monitor your wellness program, see how you are managing in daily life, and identify new concerns.
This partnered approach between physical therapy and wellness has been shown to dramatically improve the health and wellness of people with neurological conditions. Progress can continue to be made even years after a stroke due to adaptive neuroplasticity.2,3 Neuroplasticity is how your brain can re-wire after an injury or stroke. By using specific principles with your physical therapist, you can encourage your brain to continue to make new pathways and relearn movements.
Don’t let a stroke rob you of the activities you love! As a Neurological Physical Therapist (and Certified Stroke Rehab Specialist), I have a passion for promoting health and wellness for my neuro patients and I encourage you to develop a PT/Wellness Cycle. If you have any questions or want help getting started feel free to email me at gmyers@hartzpt.com or call me for a FREE phone consultation at 717.735.8880. To learn more about our stroke PT services click the button below.
REFERENCES:
1. Rafferty MR, Held Bradford EC, Fritz S, et al. Health Promotion and Wellness in Neurologic Physical Therapy: Strategies to Advance Practice. Journal of Neurologic Physical Therapy. 2021;46(2):103-117. doi:10.1097/npt.0000000000000376
2. Moheb Costandi. Neuroplasticity. The Mit Press; 2016.
3. Forrester LW. Exercise-mediated locomotor recovery and lower-limb neuroplasticity after stroke. The Journal of Rehabilitation Research and Development. 2008;45(2):205-220. doi:10.1682/jrrd.2007.02.0034

