 You are NOT Alone!
You are NOT Alone!
Welcome to HARTZ NeuroRehabilitation
Specialized Neurological Physical, Occupational and Aquatic Therapy for a Better Tomorrow
At HARTZ PT we understand that neurological conditions can affect every part of your life—mobility, confidence, and independence. Our mission is to help you move forward with expert 1-on-1 care, personalized treatments, and unwavering support.
Serving individuals and families across Lancaster County, we provide specialized physical, occupational, and aquatic therapy designed to meet the unique challenges of neurological conditions. Whether you’re recovering from a stroke, managing Parkinson’s disease, multiple sclerosis, a traumatic brain injury, or another diagnosis, our compassionate team is here to guide your journey every step of the way.
We also recognize the vital role caregivers play. That’s why we offer education, encouragement, and resources to empower and support those walking beside you.
At HARTZ, your recovery is our priority—at your pace, with your goals, and for your future.
Why Choose Us?
- Individualized, goal-oriented treatment plans
- One-on-one sessions in a calm, supportive environment
- State-of-the-art equipment and progressive therapy techniques
- Activities of Daily Living (ADL’s) practice room
- Empowering education and home exercise programs
- Support for both you & your caregivers
- Warm water aquatic therapy to improve mobility, reduce pain, and enhance balance.
Our Neurological Therapy Program Specializes in Treating Patients with the Following Disorders:
- Stroke (Cerebral Vascular Accident CVA)
- Traumatic brain injury (TBI)
- Amputation
- Spinal cord injury (SCI)
- Parkinson’s Disease
- Multiple Sclerosis
- Mild Brain Injury/Concussion
- Guillain-Barre Syndrome
- Peripheral Neuropathy
- Vestibular Disorders
- Balance Disorders
- Dystonia
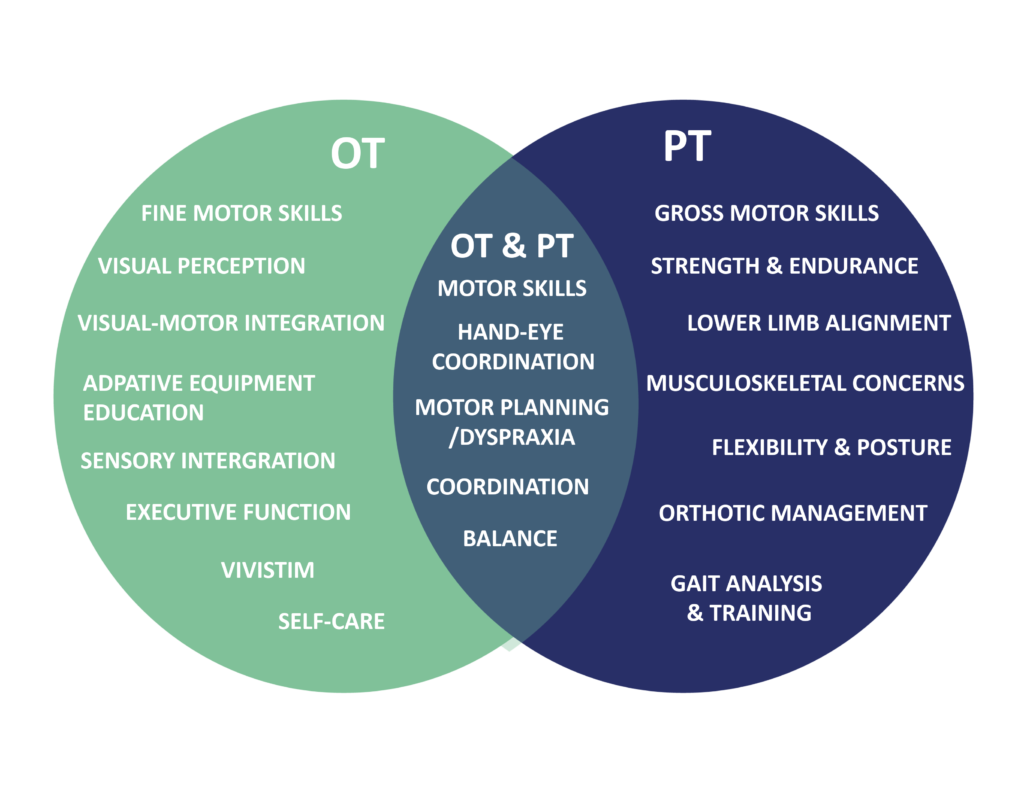
Neuro PT focuses on movement, balance, and mobility.
Neuro OT focuses on daily tasks, function, and independence.
Together? A more complete recovery.
Physical Therapy
People with neurological disorders often stop doing activities they love because it is more challenging to move, but it’s important to remember when we don’t use it….we lose it! Our PT’s have years of experience treating patients with a variety of neurological conditions. Their passion and creativity in the clinic ensure progress even with the most complicated diagnoses.
Our team can help you with the following:
- Reducing Fatigue
- Advancing Stability & Coordination
- Increasing Endurance
- Improving Posture & Balance
- Gait Training
- Practicing Transfers
- Regaining Motor Control in Arms and Legs
- Decreasing Chronic Pain & Neuropathy
- Vestibular Training
- Trunk Control / Core Stabilization
- Equipment Evaluation
Treatment may include:
- Trialing AFOs to determine the best fit to improve walking speed and safety.
- Personalized moderate to high intensity aerobic training that mobilizes neural mechanisms in the brain which create new pathways to help movement and muscle activation.
- Functional Electrical Stimulation to increase muscle recruitment during training which can improve both walking with foot drop and movement after Botox injections.
- Use of LiteGait to relearn basic walking skills, increase strength and endurance, and
promote neuroplasticity. - PNF training to improve gait and increase coordination of movements.
- Use of external verbal & visual cues during movement exercises to improve balance and overall motor performance.
Occupational Therapy
 At HARTZ PT, our occupational therapy team is here to help you feel more confident and capable in your daily life. If you or a loved one is recovering from a stroke, living with Parkinson’s, MS, or another neurological condition, we’re ready to meet you where you are and walk alongside you as you regain independence.
At HARTZ PT, our occupational therapy team is here to help you feel more confident and capable in your daily life. If you or a loved one is recovering from a stroke, living with Parkinson’s, MS, or another neurological condition, we’re ready to meet you where you are and walk alongside you as you regain independence.
Our goal is simple: help you do the things that matter most—whether that’s cooking a meal, getting dressed with ease, returning to work, or enjoying your favorite hobby.
How We Help:
- Personalized Goals: We focus on what’s meaningful to you
- Cognitive Support: Strategies for memory, focus, and problem-solving
- Arm & Hand Therapy: Building strength, coordination, and control
- Daily Task Practice: From brushing your teeth to navigating your kitchen, we work on real-life skills
- Tools & Tips: Recommendations for adaptive equipment and simple home modifications
- Caregiver Involvement: We include your support system every step of the way
With kindness, encouragement, and expert care, we’ll help you find new ways to move through life with more ease, safety, and joy.
Treatment May Include:
- Fine Motor Skill Training – Activities to improve hand function and coordination
- Cognitive Exercises – Memory games, sequencing tasks, and problem-solving strategies
- ADL (Activities of Daily Living) Practice – Hands-on support for dressing, bathing, grooming, and eating
- Energy Conservation & Fatigue Management – Helping you pace yourself and maintain independence
- Upper Extremity Strengthening – Exercises to improve arm and hand strength and range of motion
- Visual-Perceptual Training – Enhancing visual tracking, spatial awareness, and depth perception
- Home Safety Assessments – Identifying potential risks and suggesting modifications
- Adaptive Equipment Training – Learning to use tools that make daily life easier and safer
- Sensory Integration Activities – Especially helpful for those with brain injuries or sensory processing challenges
- One-on-One Education & Support – For patients and caregivers navigating new routines
Aquatic Therapy
 Our aquatic therapy program offers a safe, low-impact way to improve movement, balance, and strength—especially for those living with neurological conditions like stroke, Parkinson’s disease, multiple sclerosis, and brain or spinal cord injuries.
Our aquatic therapy program offers a safe, low-impact way to improve movement, balance, and strength—especially for those living with neurological conditions like stroke, Parkinson’s disease, multiple sclerosis, and brain or spinal cord injuries.
The water’s natural buoyancy reduces the effects of gravity, allowing you to move more freely with less pain and fear of falling. It’s an ideal environment for rebuilding confidence while working on mobility, coordination, and endurance.
Whether you’re recovering from a recent event or managing a long-term diagnosis, our one-on-one aquatic therapy sessions are guided by our experienced aquatic therapist who understands your condition and cares about your goals. With the support of warm water and a skilled team, you’ll work toward greater independence and improved quality of life—one step (or stroke!) at a time.
Benefits of Aquatic Therapy for Neuro Patients:
- Improved Balance & Walking Ability
- Reduced Muscle Stiffness & Spasticity
- Increased Strength Without Overexertion
- Gentle Cardiovascular Conditioning
- Relaxation & Pain Relief
- Boosted Confidence in Movement
Treatments May Include:
- Gait Training in Water
Practice walking in a safe, supported environment to improve stride, posture, and stability. - Balance & Core Stability Exercises
Use of water resistance and floatation tools to safely challenge your balance and strengthen your core. - Gentle Strengthening
Targeted movements to improve muscle control and endurance—without putting stress on joints. - Range of Motion Activities
Assisted stretches and guided movement patterns to maintain or improve flexibility and reduce stiffness. - Neuromuscular Re-education
Re-teaching your body how to move correctly using repetitive, functional tasks in the water. - Coordination & Motor Planning Drills
Fun, functional activities that help reconnect brain and body for smoother, more purposeful movement. - Breathing & Relaxation Techniques
Calm the nervous system, improve breath control, and reduce anxiety through focused, gentle movement. - Use of Aquatic Equipment
Including pool noodles, resistance paddles, steps, toys and flotation devices—customized to your comfort and goals.
Regain Control. Restore Confidence.
We believe in the body’s potential to adapt, improve, and thrive. With the right therapy, support, and encouragement, meaningful recovery is possible. No matter where you are on your journey, we’re here to help you take the next step.
Our Therapists:
 Jamie Hreniuk, DPT, is a physical therapist with a strong clinical focus in neurologic rehabilitation, working with patients across the lifespan—from adolescents to older adults. Her experience includes treating complex neurologic conditions such as spinal cord injuries (including ventilator-dependent cases), strokes, brain injuries, Parkinson’s disease, Multiple Sclerosis, Guillain-Barré syndrome, and ALS. Jamie specializes in creating individualized treatment plans that incorporate cutting-edge rehab technologies like body weight support systems, functional electrical stimulation, and virtual reality. She collaborates closely with interdisciplinary teams and families to ensure safe transitions and meaningful recovery at every stage of care.
Jamie Hreniuk, DPT, is a physical therapist with a strong clinical focus in neurologic rehabilitation, working with patients across the lifespan—from adolescents to older adults. Her experience includes treating complex neurologic conditions such as spinal cord injuries (including ventilator-dependent cases), strokes, brain injuries, Parkinson’s disease, Multiple Sclerosis, Guillain-Barré syndrome, and ALS. Jamie specializes in creating individualized treatment plans that incorporate cutting-edge rehab technologies like body weight support systems, functional electrical stimulation, and virtual reality. She collaborates closely with interdisciplinary teams and families to ensure safe transitions and meaningful recovery at every stage of care.
You may reach Jamie at 717.735.8880 or jhreniuk@hartzpt.com.
 Kailey Kelly, DPT is passionate about neuro and vestibular rehabilitation. She has specialized in one-on-one treatment of patients with a wide range of neurological and vestibular conditions—from stroke and traumatic brain injury to post-concussion recovery and balance disorders.
Kailey Kelly, DPT is passionate about neuro and vestibular rehabilitation. She has specialized in one-on-one treatment of patients with a wide range of neurological and vestibular conditions—from stroke and traumatic brain injury to post-concussion recovery and balance disorders.
She takes pride in providing personalized, evidence-based care using tools like High Intensity Gait Training and advanced vestibular diagnostics, including self-developed 3D models. Collaboration is key to her approach—she regularly works with occupational therapists, speech-language pathologists, and other healthcare professionals to ensure the best outcomes for her patients. Kailey is dedicated to helping her patients achieve their goals.
You may reach Kailey at 717.735.8880 or kkelly@hartzpt.com.
 Emily Beck, OTR/L our resident occupational therapist (OT) is driven by the energy that comes from progress—whether it’s a major breakthrough or a small, meaningful step forward. Seeing patients and their families recognize improvement is a powerful reminder of why the work matters. Each milestone, no matter the size, is a testament to the dedication, collaboration, and resilience shared throughout the therapeutic journey.
Emily Beck, OTR/L our resident occupational therapist (OT) is driven by the energy that comes from progress—whether it’s a major breakthrough or a small, meaningful step forward. Seeing patients and their families recognize improvement is a powerful reminder of why the work matters. Each milestone, no matter the size, is a testament to the dedication, collaboration, and resilience shared throughout the therapeutic journey.
Through a patient-centered approach and a deep commitment to functional, real-world outcomes, Emily is passionate about helping individuals regain independence, build confidence, and achieve lasting success.
You may reach Emily at 717.735.8880 or ebeck@hartzpt.com.
 Wendy Enck, PTA & our Aquatics Director focuses 1-on-1 with our aquatic therapy patients. Your aquatic rehabilitation program will always be overseen and progressed by your physical therapist, and each aquatic therapy appointment is tailored to meet the patients’ unique symptom presentation allowing for optimal progression. One patient is scheduled in the pool area at a time and monitored throughout their entire visit. With a maintained water temperature of 90-92 degrees and private changing areas with showers and towels provided, patients will be comfortable throughout their visit.
Wendy Enck, PTA & our Aquatics Director focuses 1-on-1 with our aquatic therapy patients. Your aquatic rehabilitation program will always be overseen and progressed by your physical therapist, and each aquatic therapy appointment is tailored to meet the patients’ unique symptom presentation allowing for optimal progression. One patient is scheduled in the pool area at a time and monitored throughout their entire visit. With a maintained water temperature of 90-92 degrees and private changing areas with showers and towels provided, patients will be comfortable throughout their visit.
You may reach Wendy at 717.735.8880 or wenck@hartzpt.com.
Frequently Asked Questions
What is neurorehabilitation?
Neurorehabilitation is specialized physical and occupational therapy focused on helping people recover from, manage, or adapt to conditions that affect the nervous system. This includes the brain, spinal cord, and peripheral nerves. Unlike general PT, neurorehab uses targeted techniques and specialized equipment designed specifically for neurological recovery — addressing not just strength and mobility, but also balance, coordination, cognitive function, and independence in daily activities.
What conditions do you treat?
Our neurorehabilitation program treats a wide range of neurological conditions, including:
- Stroke
- Parkinson’s disease
- Traumatic brain injury (TBI)
- Multiple sclerosis (MS)
- Spinal cord injuries
- Amputations and limb loss (including phantom limb pain and prosthetic rehab)
- Vestibular disorders and dizziness
- Peripheral neuropathy
- Post-surgical neurological recovery
If you don’t see your condition listed, contact us — our team has experience treating a broad spectrum of neurological diagnoses.
Where is your neurorehabilitation program located?
Our neurorehabilitation program is headquartered at our Lancaster West location. This office is equipped with specialized technology and space dedicated to neurological recovery, including advanced rehabilitation equipment and an activities of daily living room. Patients from all of our Lancaster County locations are welcome to receive neurorehab services there.
What specialized equipment and services are available?
Our Lancaster West neurorehab center is equipped with tools specifically designed for neurological recovery:
- LiteGait — a body weight support system that allows patients to practice walking safely, even in early stages of recovery
- Activities of Daily Living (ADL) Room — a real-life environment where patients practice essential skills like cooking, dressing, and home navigation
- Aquatic therapy — warm-water therapy that reduces stress on the body while improving strength, mobility, and coordination
- Both physical therapy (PT) and occupational therapy (OT) — so patients can receive comprehensive, coordinated care in one place
What is aquatic therapy and how does it help?
Aquatic therapy takes place in a warm-water therapy pool and uses the natural properties of water — buoyancy, resistance, and warmth — to support rehabilitation. For neurological patients, the water reduces the impact of gravity, making it possible to move and exercise with less pain and more freedom than on land. Aquatic therapy is especially beneficial for stroke recovery, Parkinson’s disease, balance disorders, and patients rebuilding strength after injury or surgery.
What is the LiteGait system?
LiteGait is a body-weight support and gait training system that suspends a portion of the patient’s weight using a harness and overhead support. This allows patients to practice walking, improve balance, and retrain movement patterns safely — even when they are not yet strong enough to bear full weight on their own. It’s a key tool in stroke and neurological recovery, helping patients build confidence and functional mobility at their own pace.
What is an Activities of Daily Living (ADL) room?
Our ADL room is a dedicated therapy space designed to look and function like a real home environment. It includes everyday fixtures and furnishings so patients can practice the tasks that matter most to them — preparing a meal, getting dressed, moving safely through a kitchen or bathroom, and more. This hands-on practice in a realistic setting helps bridge the gap between therapy and real life, so patients are better prepared when they return home.
Do I need a referral to start neurorehabilitation?
In many cases, you can begin physical therapy in Pennsylvania without a physician referral — this is known as direct access. However, some insurance plans require a referral or prior authorization for coverage. Call us first and we’ll figure it out together.
Will my insurance cover neurorehabilitation?
Most major insurance plans — including Medicare, Medicare Replacement Plans, and commercial insurers — cover physical and occupational therapy when it’s medically necessary. Neurorehabilitation generally meets that standard, though coverage details vary depending on your specific plan.
Before your first visit, we’ll verify your benefits and let you know what to expect, including any copays, deductibles, or visit limits that may apply. If prior authorization is required, we’ll handle that process on your behalf.
We believe cost shouldn’t be a barrier to care. If you have questions or concerns about coverage, call us and we’ll walk through your options together.
Will I work with both a physical therapist and an occupational therapist?
It depends on your individual needs and goals. Some patients benefit from PT alone, while others need the combined expertise of both PT and OT. During your initial evaluation, your therapist will assess your functional abilities and recommend the most appropriate plan of care. Because we offer both disciplines at Lancaster West, coordination between your care team is seamless.
What can I expect at my first neurorehabilitation appointment?
Your first visit is an evaluation — a chance for your therapist to get to know you, understand your history, and figure out the best path forward together.
They’ll review your medical history and any relevant records, ask about your symptoms, and talk with you about what you most want to get back to doing. From there, they’ll conduct a hands-on assessment of your strength, balance, coordination, mobility, and functional abilities.
By the end of the visit, you’ll have a personalized treatment plan built around your diagnosis and your goals — not a generic protocol.
Plan for about 60 minutes. To make the most of your time, it helps to bring:
- Your insurance card and photo ID
- Any referral or physician orders, if you have them
- A list of current medications
- Any relevant imaging or medical records (MRI, CT, discharge paperwork, etc.)
If you’re unsure what to bring, just call us ahead of time — we’re happy to help you prepare.
How long does neurorehabilitation take?
Every patient’s recovery is different. The length and frequency of your program depends on your diagnosis, the severity of your condition, your goals, and how your body responds to treatment. Some patients see meaningful progress in a few weeks; others benefit from longer-term ongoing care. Your therapist will regularly reassess your progress and adjust your plan accordingly, and we’ll always communicate openly with you and your referring physician.
Is it too late to benefit from neurorehabilitation if my injury or diagnosis was years ago?
No. While earlier intervention often yields faster results, the brain and nervous system retain the ability to adapt and rewire — a principle known as neuroplasticity — throughout life. Many patients make meaningful gains even years after a stroke, injury, or diagnosis. If you’ve been told there’s nothing more that can be done, we encourage you to come in for an evaluation. Our team is experienced in working with patients at all stages of recovery.

